MYOPIA AND HYPEROPIA OPERATION IN BARCELONA
Myopia and Hyperopia
What are myopia and hyperopia?
Myopia is a refractive defect that appears as a consequence of the elongation of the eyeball. This elongation of the eyeball gives the eye the characteristics of a magnifying glass, that is:
- Very poor distance vision which starts to become apparent from a few metres away.
- Good near vision, which leads to a tendency to move closer to objects.
Hyperopia is just the opposite. The eyeball is smaller than usual, causing it to focus behind the retina, which leads to poor near vision and good distance vision.
Astigmatism is a refractive error whereby, regardless of the length of the eye, the image refracted by the cornea is in an oblique plane with respect to the retinal plane due to an anatomical alteration of the cornea. This causes a distortion of the images.
SURGERY FOR MYOPIA AND HYPEROPIA IN BARCELONA
Both hyperopia and myopia, together with astigmatism, are what are known as refractive defects. To eliminate them, at Clínica Castanera we basically work with two refractive surgery techniques in Barcelona:
- Collamer lens.
- Laser (LASIK or PRK).
Both techniques are totally safe and very fast. So much so that the same day of the intervention the patient can go home on their own, and the next day they can start to lead a practically normal life, without the need to wear glasses or contact lenses of any kind. The choice of one surgery or another depends mainly on the anatomical characteristics of the eye, which will be determined by a battery of diagnostic tests at our practice.
CHOOSE YOUR OPERATION FOR MYOPIA AND HYPEROPIA IN BARCELONA
What is a collamer lens?
One of its main characteristics is that it is very flexible. This allows it to be folded, or rather rolled up, so that it can be inserted into the eye through a minimal incision. It is also capable of correcting very high prescriptions, making it a great choice for patients with very high refractive errors.

Why choose this kind of intervention?
What tests are performed during the pre-operative period?
A whole battery of diagnostic tests are carried out to determine the patient’s prescription and to find out exactly what type of lens and what power it should have. It should be borne in mind that this type of lens, in most cases, is ordered and manufactured specifically for each individual patient.
But of all the tests, one of the most important is biometry. This is a test in which we can measure exactly the space between the iris and the crystalline lens. This measurement is extremely important because it will be decisive in determining whether or not the space is sufficient to accommodate the collamer lens that will be placed in this space.
What if I am not a candidate for collagen lens implantation?
What does the intervention involve?
As mentioned above, the lens can be folded back on itself. This allows it to be introduced into the eye through a minimal incision (2.2mm) and unfold inside.
Dduring your myopia and hyperopia surgery in Barcelona with our doctor, the lens is positioned behind the iris and is held in place by the four haptics located on the edges.
How long does the procedure take?
The procedure takes no more than 10 minutes per eye as no internal structures of the eye have to be altered, the lens simply has to be positioned properly behind the iris.
Will I feel any pain?
No, you will not feel any pain. Our myopia and hyperopia surgery in Barcelona is performed under local anaesthesia and a light sedation that allows the patient to be totally relaxed, in a kind of sleep, and the eye completely anaesthetised.
Can they put me completely to sleep so that I'm not aware of anything?
When will I start to see properly?
This is one of the best parts of having this surgical technique, as patients begin to see more than satisfactorily as soon as the operation is over. Many of them are still in the operating theatre and are surprised at how well they can see without glasses.
In any case, it should be borne in mind that full recovery may take a few days, no more than a week.
ALL REFRACTIVE SURGERY OPTIONS IN BARCELONA
This technique consists of altering the anatomical characteristics of the cornea by permanently modifying its curvature, and therefore its dioptric power. The remodelling is carried out in a very precise and controlled manner by vaporising the corneal tissue. Laser pulses polish the surface of the cornea with great precision until the refractive error is eliminated.
What is the difference between LASIK and PRK?
The choice between one technique or the other is based solely on medical criteria.
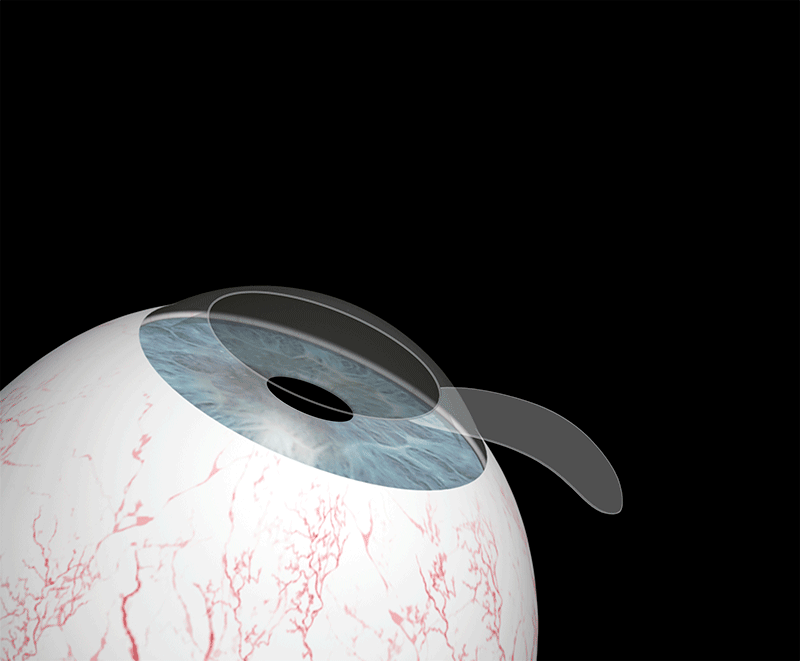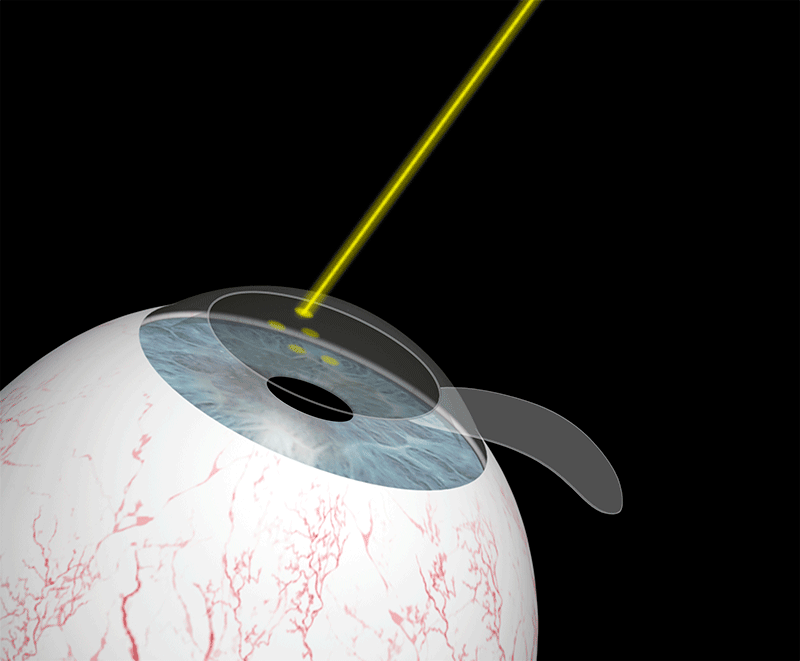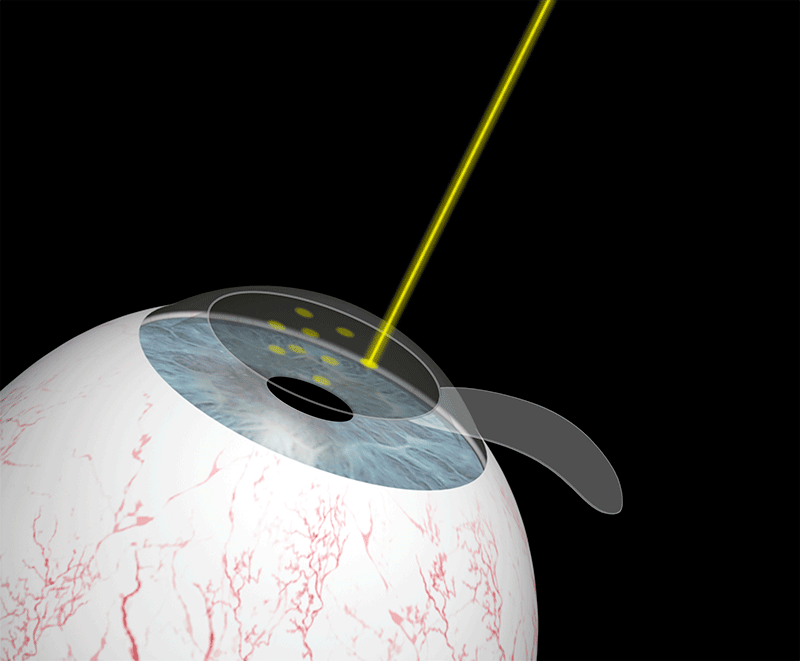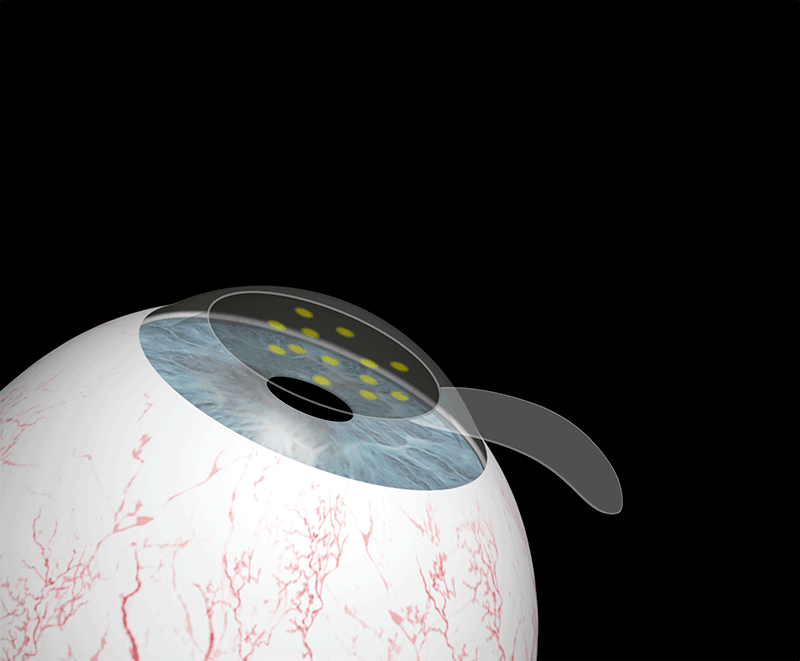
How do I know if I can undergo laser surgery?
What tests are performed preoperatively?
Por lo tanto, es imprescindible saber si nuestra córnea es lo suficientemente gruesa para soportar esta sustracción.
En cualquier caso se trata de pruebas no invasivas y rápidas en las que, principalmente el paciente tan solo deberá mirar una luz y permanecer unos segundos con el ojo abierto.
What if I am not eligible for this technique?
If the thickness of the cornea is not thick enough to support the removal of tissue required for our prescription, there are only two alternatives: continue wearing glasses or contact lenses or opt for collamer lens implantation surgery.
How long does the procedure take?
Will I feel any pain?
No. Before the operation, the patient is given a sublingual relaxant to provide a relaxed state. In addition, drops of anaesthetic eye drops are instilled into the eye so that it is completely asleep before being manipulated.
When will I start to see well after surgery?
This is precisely another of the differences between these two techniques: while recovery with LASIK is more immediate (more than acceptable vision is achieved the following day), with PRK it takes between 7 and 15 days for vision to stabilise. This is due to the fact that the epithelium must regenerate completely and during this time the vision may fluctuate until it reaches its optimum state.
Contact us

M - T. 9:00 a 14:00 | 15:00 a 19:00
F. 9:00 a 14:00



